Public Health Initiatives: Address public health initiatives, including awareness campaigns, education, and resources in regard to non-opioid treatment practices
Allison Oteju, Medical Affairs Intern
Pain management is changing, and for many patients, it’s a positive shift. As research grows and healthcare teams learn from real‑world experience, the focus is moving toward treatments that ease pain while supporting safe, healthy recovery.1
One of the biggest changes is the increasing use of non‑opioid options for sudden muscle and joint pain. Whether it’s a sprain, strain, or another quick injury, patients and clinicians are looking for ways to get relief without the risks that can come with opioids.1
The idea is simple: the best pain care helps you recover faster, stay safe, and avoid long‑term problems.
The Public Health Imperative: Reducing Opioid Dependency
In the late 1990s and early 2000s, opioid prescribing expanded significantly. Over time, rising misuse and overdose rates prompted action from organizations such as the Centers for Disease Control and Prevention and the U.S. Food and Drug Administration.4
Updated national guidelines now emphasize:
- Non-pharmacologic therapies first
- Non-opioid pharmacologic options when medication is needed
- Short-term, lowest-effective dosing strategies
- Patient-specific risk assessment
Multimodal Non-Opioid Therapy: How It Works
Acute musculoskeletal pain is now widely recognized as a condition where opioids are rarely the only option and where nonpharmacologic strategies (ice, heat, rest, elevation, movement-based therapy) plus nonopioid medications (eg, topical/oral NSAIDs, acetaminophen) are commonly appropriate.⁵
Many clinicians and health systems also use a multimodal analgesia mindset, combining approaches that address inflammation, function, and pain signaling to support symptom relief and recovery while reducing opioid exposure.2
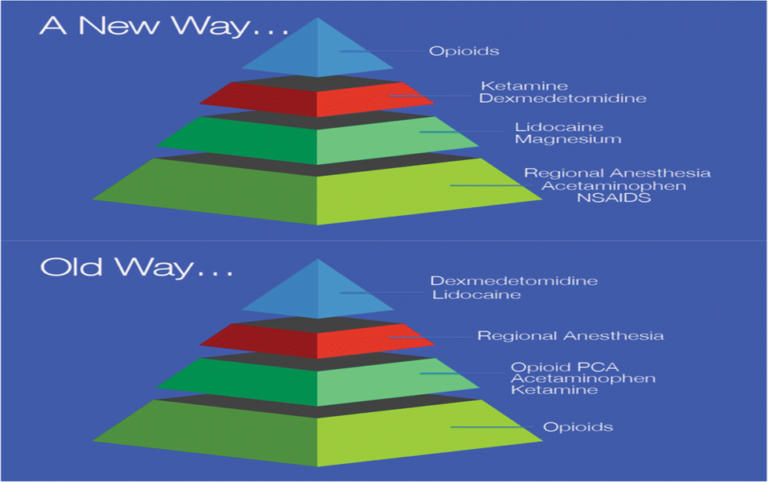
New paradigm in analgesia management. Koepke et al. Perioperative Medicine. Published July 2018.https://www.researchgate.net/publication/326159168
Public Health Efforts Supporting Safer, Non‑Opioid Pain Care
1. Helping Clinicians Choose Safer Options
Health programs and professional guidelines encourage clinicians to:¹ ²
- Use medications such as ibuprofen or naproxen when appropriate
- Consider non-opioid alternatives before initiating opioid therapy
- Engage patients in shared decision-making
- Focus on functional improvement rather than numeric pain scores
Professional organizations support a “stepwise” approach, starting with the safest and most evidence-based therapies.²
2. Empowering Patients Through Awareness
Public health messaging encourages patients to ask informed questions, including:¹
- “Are there non-opioid treatments I can try first?”
- “What risks come with stronger pain medications?”
- “Could anti-inflammatory therapy or short-term muscle relaxation help manage this?”
Education initiatives aim to improve understanding of risks, benefits, and safe medication practices.¹
3. Improving Safety Through Monitoring and Stewardship
Prescription Drug Monitoring Programs (PDMPs) were implemented nationwide to reduce inappropriate opioid prescribing and identify patterns of misuse.⁴
At the same time, healthcare teams evaluate non-opioid treatments for:
- Gastrointestinal risk
- Sedation or anticholinergic effects
- Drug–drug interactions
- Patient-specific health conditions
Public health initiatives emphasize that safe care requires individualized treatment planning and ongoing reassessment.¹
Looking Ahead
Public health efforts are moving toward:
- More personalized prescribing
- Better tools to match treatments to patient risks
- Stronger real-world safety monitoring
- Ongoing clinician education
- Clear, patient-centered communication
The future of pain care will blend medications, rehab, and personalized treatment to help people recover safely and effectively.
References
- Dowell D, Ragan KR, Jones CM, Baldwin GT, Chou R. CDC clinical practice guideline for prescribing opioids for pain—United States, 2022. MMWR Recomm Rep. 2022;71(3):1-95.
- Qaseem A, McLean RM, O’Gurek D, et al. Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical guideline from the American College of Physicians. Ann Intern Med. 2017;166(7):514-530.
- Chou R, Deyo R, Friedly J, et al. Nonpharmacologic therapies for low back pain: a systematic review for an American College of Physicians clinical practice guideline. Ann Intern Med.2017;166(7):493-505. doi:10.7326/M16-2459
- Dart RC, Surratt HL, Cicero TJ, et al. Trends in opioid analgesic abuse and mortality in the United States. N Engl J Med.2015;372(3):241-248. doi:10.1056/NEJMsa1406143
- Centers for Disease Control and Prevention. Nonopioid therapies for pain management. Updated January 31, 2025. Accessed February 26, 2026
The information provided is for general informational and educational purposes only. It is not intended to serve as medical advice, diagnosis, or treatment. The content is written by a licensed pharmacist and reflects general knowledge and expertise in the healthcare field, but it is not a substitute for professional medical advice from a qualified healthcare provider.
Always consult your physician, pharmacist, or other qualified healthcare professional before starting, stopping, or modifying any medication, treatment, or health regimen. Individual health conditions and needs vary, and only a healthcare professional can provide personalized advice tailored to your specific situation.
While we strive to ensure the accuracy and currency of the information presented, medical knowledge is constantly evolving, and errors or omissions may occur. The blog’s content does not cover all possible uses, precautions, side effects, or interactions of medications or treatments. Reliance on any information provided is solely at your own risk.
Links to external websites or resources are provided for convenience and do not imply endorsement or responsibility for their content.






